Expert personalised treatment specialising in the management of knee and shoulder disorders, trauma and sporting injuries.
Expert personalised treatment specialising in the management of knee and shoulder disorders, trauma and sporting injuries.
Specialist orthopaedic services to help you achieve better bone and joint health and optimal performance.
Dr Graeme Brown is an Australian based and trained orthopaedic surgeon providing consulting and surgical services for patients in Geelong and the surrounding regions.
A passionate and driven sports person, Dr Brown completed his orthopaedic training at the University of Melbourne in 1994 through the Australian Orthopaedic Association.
Committed to excellence in care and outcomes, he then undertook additional training in leading international orthopaedic centres around the world.
This included fellowship training for joint replacement surgery in Exeter in the UK, one of the world’s leading joint replacement centres. Then training based on the treatment and management of sports related orthopaedic conditions of joints and soft tissue affecting the knee and shoulder, at Salt Lake City’s Orthopaedic Sports Hospital in the USA.
In 1996, Dr Brown returned to Australia and established a practice where he has continued to provide specialist orthopaedic services with a focus on conditions affecting the knee and shoulder. For his patient’s convenience, consulting services are provided at Geelong Orthopaedics in Geelong and surgical services at St John of God Geelong Hospital and the Epworth Geelong hospital.
Driven for better patient outcomes he continues to provide expert non-interventional and interventional treatment and care for all patients requiring joint replacement surgery of the knee and shoulder, for the management of soft tissue conditions affecting the knee and shoulder and for the treatment of trauma and sporting injuries of the knee and shoulder.

Conditions
Dr Brown specialises in the management and treatment of a range of conditions including:
Meet Dr. Brown
Dr Brown has successfully treated many patients with rotator cuff injuries and is knowledgeable in the latest non-surgical and surgical treatments.
Call us on (03) 5223 3151 Book an appointment today.




PATIENT-CENTRIC, EVIDENCE-BASED APPROACH
Utilising a patient-centric, evidence-based approach, spending time with and getting to know his patients is an important part of Dr Brown’s treatment philosophy.
Better Treatment Outcomes
Dr Brown and his team are focused on ensuring their patients are treated with the most up to date methods of the highest standard in a friendly, professional, and caring environment.
Specialised Treatment Programs
Dr Brown’s expertise lies in the management of orthopaedic conditions, implementing the latest state-of-the-art surgical techniques and non-surgical treatment methods through the adoption of gold standard developments from around the world. Dr Brown’s expertise lies in the management of orthopaedic conditions, implementing the latest state-of-the-art surgical techniques and non-surgical treatment methods through the adoption of gold standard developments from around the world.
Clear and Concise Treatment Plan
Throughout his career as an orthopaedic surgeon, Dr Brown has cared for many patients and understands that seeing a specialist can be intimidating. During your consultation, Dr Brown will perform a comprehensive assessment to identify the best treatment options for you. The treatment plan is designed to empower you to play an active role in your recovery, enabling you to return to a healthy lifestyle no longer affected by diminished mobility.












Best Fit Blog
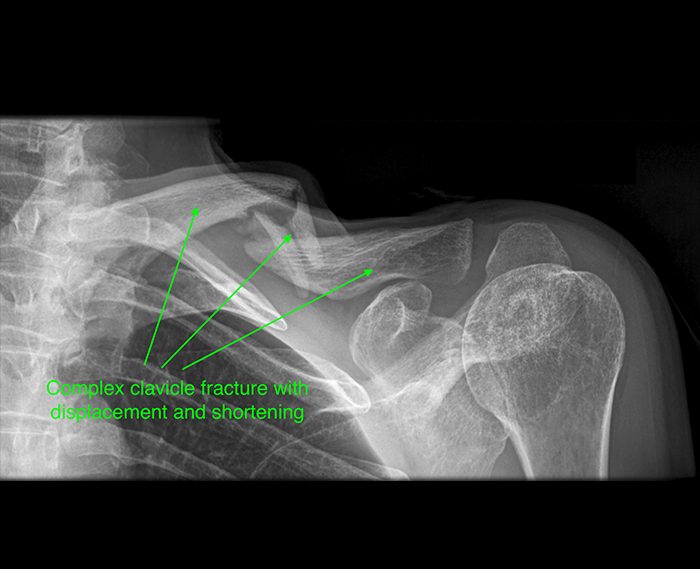

Common Cycling Shoulder Injuries in Spring & Summer
As we move into Spring and Summer, with warmer weather and longer days, many more people dust off and get out their bikes. There are

ACL surgery is superior to rehabilitation
As discussed previously, ACL injuries are prevalent. They are a common injury in many pivoting sports popular in Australia. These “at-risk” sports include Australian Rules


Common Ski Injuries -including ACL tears
With winter on our doorstep, many people will head to the Australian snowfields. According to the Australian Ski Areas Association, there were over 2,500,000 “skier”

