KNEE ARTHRITIS
The knee joint is commonly affected by arthritis. Because it is a significant weight-bearing joint with a pivotal role in may activities, it can have a considerable impact on a person’s life. Arthritis is a progressive disease. However, it comes on over years and decades. When the cartilage is completely lost, the person may reach the stage of having “bone on bone”.
Many conditions lead to cartilage damage and osteoarthritis. However, most cases are idiopathic, which means that there is no specific cause. There is probably a genetic component to this idiopathic variety and that joints other than the knee are commonly involved (hips and hand). Knee injuries can damage the cartilage. Injuries include fractures that extend into the joint and fractures of the leg bones that heal in a “crooked” position. Ligament and meniscal tears can also predispose to arthritis. There are also a group of diseases that cause inflammation of a joint such as Rheumatoid Arthritis that can lead to cartilage damage. Arthritis is commoner as a person ages, but it is not an inevitable consequence of ageing.
SYMPTOMS OF KNEE ARTHRITIS
- Swelling
- Deformity
- “Mechanical” symptoms such as catching
- Loss of movement, including the inability to straighten the leg
- entirely
- Limp
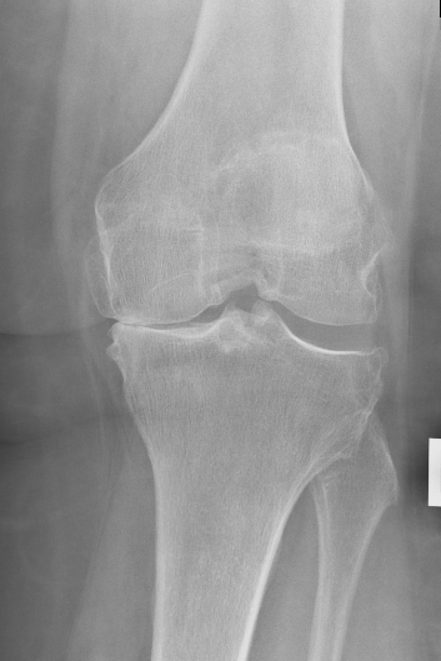
KNEE ARTHRITIS DIAGNOSIS
The diagnosis of osteoarthritis of the knee can be made based on the person’s age, symptoms and the findings when a doctor examines your knee.
However, imaging of the knee is required to confirm the diagnosis. Although the severity of the symptoms is vital in assessing the stage of the arthritis, imaging plays an important role too. X-Rays, especially weight-bearing X-Rays, show characteristic changes. The most significant changes are a reduced gap between the two bones (indicative of the extent of cartilage damage) and the presence of bone spurs (osteophytes) that project out from the bones. An MRI is not required to confirm the presence of arthritis but will demonstrate characteristic features.
It is essential to know that as yet the cartilage damage cannot be repaired. The cartilage loss is progressive but occurs over the years to decades. As mentioned above, and it needs to be stressed enough, the pain from the arthritis is intermittent.
Call us on (03) 5223 3151 Book an appointment today.

