Knee replacement surgery has revolutionised the treatment of end-stage osteoarthritis. The first knee replacement was performed in the 1960s but was popularised in the USA in the early 70s. Currently, in Australia, over 60000 knee replacements are performed a year.
Many factors contribute to a good outcome after knee replacement surgery. The timing of surgery is critical; too early in the disease and the risk-benefit works against you, but if you have surgery too late in the course of the disease, chronic pain, stiffness and deformity can work against you.
Patients must have the right attitude to their rehabilitation. I see it as a contract: I’ll do my best as the surgeon, and the patient needs to put in the hard work and be responsible for their rehabilitation.
The technical factors in the surgery are essential. The history of knee replacement surgery has been progressive advancements in placing the knee replacement components as accurately as possible. The first generation of knee replacements were inserted in what now looks like a reasonably crude fashion. With better instrumentation and tools, a surgeon could put the components consistently in a good position.
The next significant change came with the advent of computer navigation systems. Computer navigation improved the accuracy of the bone cuts, which led to a more precise and reproducible alignment of the knee replacement. This precision produced fewer complications and improved pain and functional outcomes.
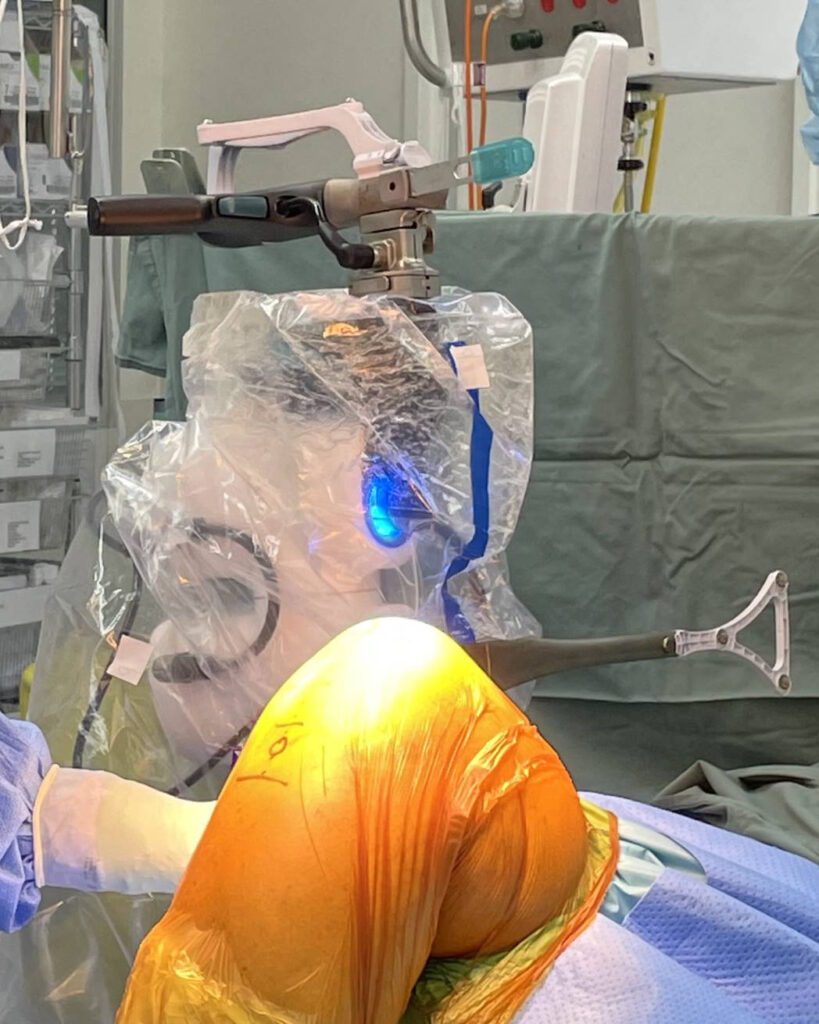
Most recently, robotic-assisted surgery has been the next major advancement. For example, robotics has improved the navigation system’s accuracy and the precision of knee replacements. I stated above that it’s called “robotic-assisted” surgery. The robot helps plan the bone cuts and assists in performing the cuts accurately, but the surgeon still has ultimate control of the system. It is a new and exciting step in advancing knee replacement surgery. And it’s good to be part of this evolution in knee replacement surgery, with expected improved results.
To book an appointment with Dr. Brown, please refer to the information found on this page.